Successful murine model of dermatomyositis reveals underlying immune system involvement
April 11, 2024
Researchers from Tokyo Medical and Dental University (TMDU) have developed a murine model for a highly progressive disease called “anti-MDA5 antibody-positive dermatomyositis”, providing insights into underlying biological mechanisms and aiding treatment
Tokyo, Japan – Some diseases involve autoimmune reactions, when the body begins to attack its own cells and proteins. The biological mechanisms underlying these diseases are often unknown, making treatment challenging. Now, a group at TMDU has created a murine model for a disease known as “anti-MDA5 antibody-positive dermatomyositis”. Use of this model has allowed them to identify components of the immune system that are vital in disease development, with implications for future treatments.Dermatomyositis is a member of a disease group known as idiopathic inflammatory myopathies, which cause typical rashes and muscle weakness, leading to disability and premature death. As part of the normal immune response, the body produces proteins known as antibodies, specific to individual “antigens”, or foreign substances. However, autoimmune reactions involve the abnormal production of antibodies to human proteins, called “autoantibodies”. Anti-MDA5 antibody-positive dermatomyositis involves the production of autoantibodies against the protein MDA5, causing rashes and lung inflammation and fibrosis, called interstitial lung disease (ILD). This often progresses very rapidly with a high mortality rate, and current anti-inflammatory treatments are ineffective.
“To develop a model of this disease in mice, we first triggered the production of anti-MDA5 autoantibodies,” explains lead author of the study Dr. Yuki Ichimura. “This resulted in the development of some lung inflammation but not full ILD.” Because MDA5 is involved in the body’s response to certain viruses, the team then mimicked a viral infection in the lungs. The mice producing anti-MDA5 antibodies developed significant lung inflammation and fibrosis, emulating the pathogenesis seen in human patients, successfully modeling the disease.
The researchers then analyzed the specific immune responses occurring in the mice and investigated how these led to disease. Of the various cells involved in the immune response, they showed that cells called “CD4-positive T cells” are key for the development of ILD. Experimentally reducing the numbers of these cells lessened the lung damage observed. The involvement of these T cells is backed up by autopsy findings from the lungs of patients.
The research team went on to identify elevated levels of a signaling molecule called interleukin-6 in the murine model. “Experimental reduction of interleukin-6 levels ameliorated the development of ILD,” explains senior author Dr. Naoko Okiyama, “indicating that medical intervention targeting interleukin-6 could be a potential treatment option for ILD.”
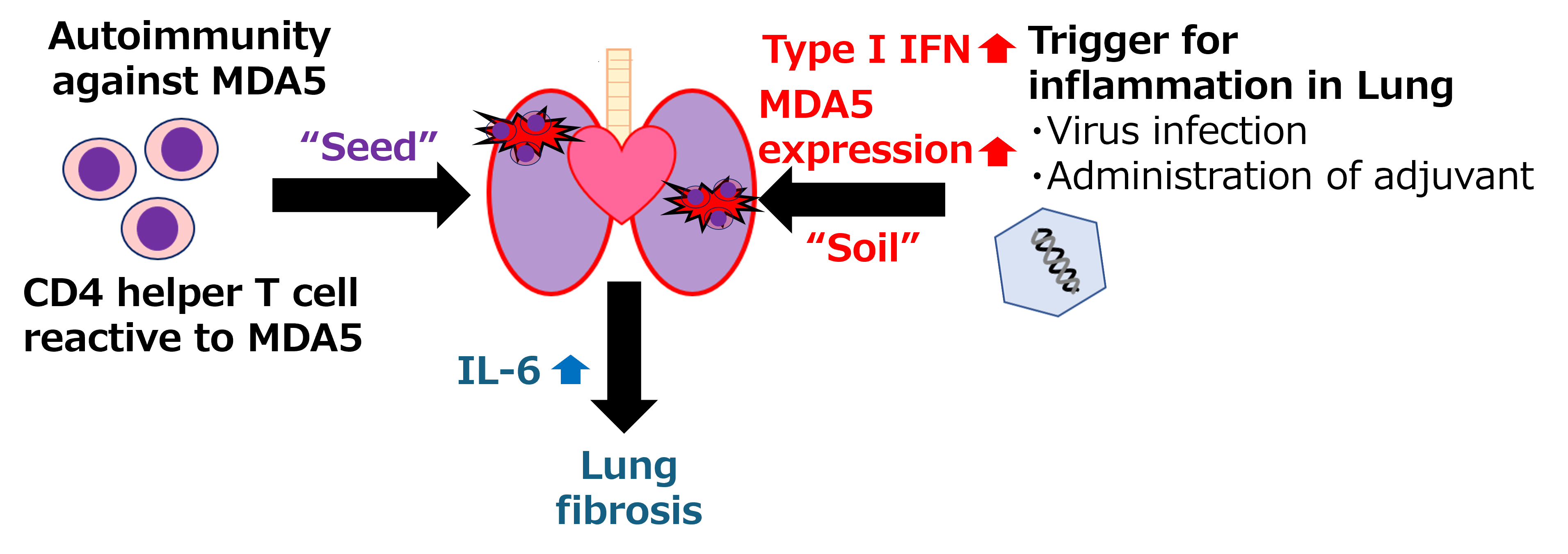
Pathogenesis in the MDA5-induced interstitial lung disease
Autoimmunity to MDA5, CD4 T cells reactive MDA5, works as 'Seed', and inducible factors like as virus infection and poly (I:C) treatment induce type I IFN upregulation and MDA5 expression on the lung and works as 'Soil'. The seed and soil work together to establish interstitial lung disease. IL-6 mediates lung fibrosis.
The murine model developed in this study provides a key tool for investigating the mechanisms underlying anti-MDA5 antibody-positive dermatomyositis, the value of which is proved by the identification of key factors in the immune system involved in this highly progressive disease. Future work enabled by this study could aid in the development of more specific and effective therapies, improving treatment and quality of life.
###
The article, “Autoimmunity against melanoma differentiation-associated gene 5 induces interstitial lung disease mimicking dermatomyositis in mice”, was published in PNAS at DOI: https://doi.org/10.1073/pnas.2313070121
YouTube: https://youtu.be/hvHLDlmO7GU?si=39XK2wsEUuuMxOKZ
###
The article, “Autoimmunity against melanoma differentiation-associated gene 5 induces interstitial lung disease mimicking dermatomyositis in mice”, was published in PNAS at DOI: https://doi.org/10.1073/pnas.2313070121
YouTube: https://youtu.be/hvHLDlmO7GU?si=39XK2wsEUuuMxOKZ
Summary
Researchers from Tokyo Medical and Dental University (TMDU) have developed a murine model of “anti-MDA5 positive dermatomyositis”, a rare, progressive autoimmune disease with a high mortality rate. This model provides a tool for understanding the underlying disease pathogenesis and identifying novel therapeutic targets. They identified components of the immune system—CD4-positive T cells and interleukin-6—as key in the development of associated lung fibrosis, and showed that intervention to reduce their levels can ameliorate disease development.
Journal Article
JOURNAL: Proceedings of the National Academy of Sciences of the United States of America
TITLE: Autoimmunity against melanoma differentiation–associated gene 5 induces interstitial lung disease mimicking dermatomyositis in mice
DOI: https://doi.org/10.1073/pnas.2313070121
TITLE: Autoimmunity against melanoma differentiation–associated gene 5 induces interstitial lung disease mimicking dermatomyositis in mice
DOI: https://doi.org/10.1073/pnas.2313070121
Correspondence to
Naoko Okiyama, Professor
Department of Dermatology,
Graduate School of Medical and Dental Sciences,
Tokyo Medical and Dental University(TMDU)
E-mail:okiy.derm(at)tmd.ac.jp
*Please change (at) in e-mail addresses to @ on sending your e-mail to contact personnels.

