High pressure tissue decellularization offers promise for tissue engineering applications
PDF Download
- Tissue decellularization

Akio Kishida
Professor of Material-based Medical Engineering at TMDU
Profile
Dr. Kishida graduated from the Faculty of Engineering at Kyoto University, where he received his MD and PhD. He became Assistant Professor in 1992, and Associate Professor in 1994 at Kagoshima University. He joined TMDU as Professor of aterialbased Medical Engineering at the Institute of Biomaterials and Bioengineering in 2004. In 2014, TMDU established the Department of Acellular Biomaterials and Regenerative Medicine and Dr. Kishida became the field manager there.
A:From the late 1990s, it has been reported that human decellularized tissue-extracellular matrix from which cellular components have been removed-works well as a substitute for living tissue. Decellularized tissue exhibits good biocompatibility, and the lack of donor cellular material minimizes the risk of graft rejection. Importantly, the removal of donor ellular material may allow for the use of animal tissue as a source for xenotransplantation into humans, so this technology has the potential to provide a high-performance scaffold for tissue engineering.
A:The main existing approach for decellularizing tissues involves using detergents. Such techniques may leave residual cytotoxic chemicals or change the mechanical properties of the tissue. We developed an alternative method of decellularizing tissues using highhydrostatic pressure (HHP, >600 MPa). The cell debris can then be removed by washing, without chemicals or detergents.
A: In vivo grafts of HHP-decellularized tissues show minimal inflammation and exhibit good long-term stability. Grafted decellularized tissues can also strongly recruit host cells, facilitating rapid integration into host tissue. An additional benefit is that HHP has a sterilizing effect: Because the treatment disrupts lipid bilayers, it can destroy pathogens such as bacteria, fungi, and some viruses.
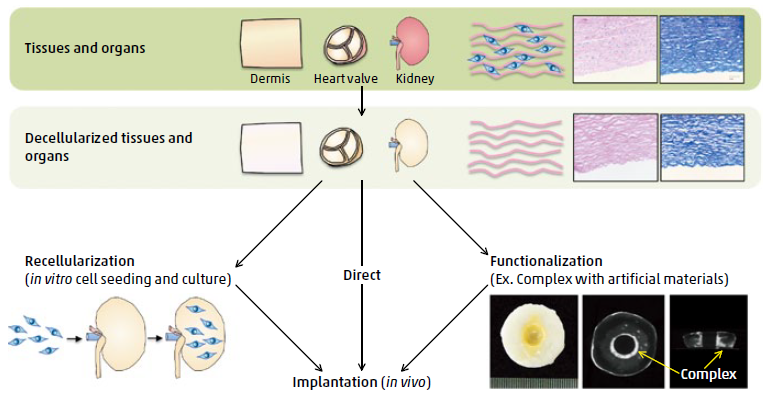
Overview of applications of decellularized tissues and organs
A: We transplanted decellularized porcine corneas into rabbits, and achieved transparent corneas that lasted for at least twelve months after transplantation.
Another challenge we tackled was developing graft materials that can function as an interface between hard and soft tissues. We have used decellularized tissues in conjunction with a synthetic polymer to develop a hybrid biomaterial. This material can function s an interface between different tissue types, or between a tissue and an implanted synthetic device.
We also explored using powders made from decellularized tissues for treating myocardial infarction in a rat model. Decellularized liver powder promoted cell integration and neovascularization both in vitro and in vivo, and suppressed myocardial necrosis.
A: We are working on regenerating bone marrow, brain, and cartilage using the relevant decellularized tissues. Decellularized tissue is emerging as superior to many artificial materials currently used in tissue engineering. We will continue working with our research partners to explore the potential of decellularized tissue.
Journal Information
Mater. Sci. Eng. C, doi: 10.1016/j.msec.2013.11.007
Tissue Engineering with Natural Tissue Matrices
Adv. Sci. Tech., doi: 10.4028/www.scientific.net/AST.76.125
The use of high-hydrostatic pressure treatment to decellularize blood vessels,
Biomaterials, doi: 10.1016/j.biomaterials.2010.01.073
Preparation and characterization of decellularized cornea using high-hydrostatic pressurization for corneal tissue engineering
Biomaterials, doi: 10.1016/j.biomaterials.2010.01.122
Effect of decellularized tissue powders on a rat model of acute myocardial infarction,
Mater. Sci. Eng. C, doi: 10.1016/j.msec.2015.07.010

